If you have LPR (silent reflux), pepsin in the throat is the root cause of almost every symptom you’re experiencing. Not the acid — the pepsin. The acid gets most of the attention because that’s what heartburn is associated with, but for LPR it’s a digestive enzyme called pepsin that is actually doing the damage.
The good news is that pepsin can be deactivated. Once it’s neutralised it cannot cause any further damage and cannot be reactivated. Understanding how to do this — and how to stop more pepsin from reaching the throat in the first place — is the foundation of managing LPR effectively.
Key Takeaways:
- Pepsin in the throat is the primary driver of LPR symptoms — not stomach acid
- Pepsin can remain dormant in throat cells for up to 24 to 48 hours after a reflux episode and be reactivated by anything acidic
- Alkaline water at pH 8.8 or above permanently and irreversibly deactivates pepsin — confirmed by Koufman and Johnston’s 2012 study
- An alkaline water throat spray is one of the most direct ways to deactivate pepsin already embedded in throat tissue
- Avoiding foods with a pH below 5 prevents dormant pepsin from being reactivated
- Gaviscon Advance (UK version) prevents more pepsin from reaching the throat in the first place
- A low acid diet addresses pepsin reactivation from the dietary side simultaneously
What Pepsin Is and Why It’s the Problem
Pepsin is a digestive enzyme produced in the stomach whose job is to break down proteins. In the stomach it’s harmless — the stomach lining has protective mechanisms designed to handle it. The problem starts when it travels somewhere it doesn’t belong.
With LPR, gaseous reflux carries pepsin all the way up past the oesophagus and into the throat, voice box and sometimes higher — into the sinuses, ears and airway. Once it reaches the throat, pepsin starts doing what it’s designed to do: break down protein. Your throat tissue is protein. This is what causes the inflammation, the burning, the constant irritation.
Here’s the part that makes pepsin particularly problematic compared to acid: pepsin can remain active in throat tissue for up to 24 to 48 hours after a reflux episode. It doesn’t clear quickly. It sits dormant in the cells of the throat lining, waiting. And if anything acidic — food, drink, even another small reflux event — comes into contact with it during that window, the pepsin gets reactivated and the damage cycle begins again.
This is why LPR symptoms can feel relentless even when you think you’re being careful. The pepsin from yesterday’s meal is still there, being reactivated by today’s coffee or orange juice.
Pepsin remains stable at neutral pH — including the typical pH of the throat (around 6.8) — which means it’s not being cleared naturally either. It sits and waits. The only thing that permanently deactivates it is exposure to something sufficiently alkaline.
Method 1: Drinking Alkaline Water
Drinking alkaline water at pH 8.8 or above permanently deactivates pepsin on contact. This is the most important thing you can do on a daily basis to manage pepsin in the throat, and it’s backed by solid research.
The key study is Koufman and Johnston (2012), published in the Annals of Otology, Rhinology and Laryngology. Their laboratory testing showed that water at pH 8.8 instantly and irreversibly denatured human pepsin — rendering it permanently inactive. The same water also had far superior acid-buffering capacity compared to regular bottled water. This is the study that established the scientific basis for alkaline water as a pepsin management tool.
Every time you drink alkaline water it passes over the throat and any pepsin it contacts is permanently deactivated. This is why I recommend making it your default water throughout the day — not an occasional supplement to your normal water intake, but a replacement for it. Every time you drink regular water at pH 6 to 7 instead, you’re missing a chance to neutralise dormant pepsin.
Aim for pH 9 or above to give yourself a comfortable margin above the 8.8 threshold. Naturally alkaline spring water is the best option — this is what the Koufman study used. A quality alkaline water filter pitcher is a more cost-effective option for daily use. For full details on choosing the right water see my dedicated alkaline water for LPR guide.
Timing matters: first thing in the morning before anything else is particularly valuable — overnight reflux during sleep means pepsin may have reached the throat, and alkaline water immediately on waking addresses this. After any meal, and especially after anything even slightly acidic, is also a good time.
Method 2: Alkaline Water Throat Spray
Drinking alkaline water helps, but the water passes through the throat quickly. For pepsin that has embedded itself deeper into throat tissue — particularly relevant for people with persistent symptoms — a throat spray allows more targeted, sustained contact with the affected area.
Dr Koufman has recommended this approach specifically for people with symptoms like excessive mucus, chronic throat clearing, voice problems, globus and chronic cough — all of which are signs of pepsin embedded in the upper throat and voice box area where a quick drink of water may not reach as effectively.
How to make the alkaline throat spray:
- Take 250ml (8oz) of alkaline water — ideally pH 9 or above
- Add half a teaspoon of baking soda and stir until fully dissolved — this raises the pH further and increases the alkaline buffering capacity
- Pour into a small personal spray bottle
- Spray 2 to 4 times into the back of the throat, breathing in gently through the mouth as you do so to help the spray reach the voice box area
When to use it: after meals, after anything acidic, before bed, and first thing in the morning. I’d suggest 3 to 4 times per day as a minimum. You can use it more often without concern — it can’t cause harm.
A few things worth knowing: make a fresh batch daily rather than storing it for multiple days. If your throat burns when you use it, that’s unusual — it may indicate alkaline reflux rather than acid reflux, in which case stop and reassess. For most people it should be neutral or soothing rather than irritating.
This method is particularly useful during a flare-up or in the early weeks of treatment when pepsin levels in the throat are high. Many people find they can reduce frequency as their symptoms improve and the throat heals.
Method 3: Avoiding Foods That Reactivate Pepsin
Deactivating the pepsin already in your throat is only half the battle. The other half is stopping dormant pepsin from being reactivated by what you eat and drink.
Pepsin is reactivated by acidity — specifically by anything with a pH below 5 coming into contact with the throat. The more acidic the food or drink, the more aggressively it reactivates the pepsin. This is why the low acid diet is so central to managing LPR — it’s not just about reducing reflux triggers, it’s about not handing the dormant pepsin in your throat the ammunition it needs to start causing damage again.
The key offenders that reactivate pepsin most aggressively are soft drinks (even diet versions), coffee, alcohol, citrus fruits and juices, tomatoes and tomato-based sauces, vinegar and vinegar-containing condiments, and anything carbonated. All of these have a pH well below 5.
It’s also worth noting that pepsin can be active up to pH 8.0 — so even foods that are mildly acidic (pH 5 to 8) can still cause some reactivation, just to a lesser degree. The threshold for avoiding foods is commonly stated as pH 5, but being conservative with pH 6 or above is better if your symptoms are still active.
For the full detailed breakdown of what to avoid and why, see my LPR foods to avoid guide.
Method 4: Gaviscon Advance — Stop More Pepsin Reaching the Throat
The methods above deal with pepsin that has already reached the throat. Gaviscon Advance (UK version) works differently — it prevents more pepsin from getting there in the first place.
When you take Gaviscon Advance after a meal, the sodium alginate it contains reacts with stomach acid to form a physical raft that sits on top of the stomach contents. This raft acts as a mechanical barrier — when reflux occurs, the raft refluxes instead of stomach acid and pepsin, protecting the oesophagus and throat from exposure.
Gaviscon Advance does not neutralise pepsin. What it does is dramatically reduce the amount of new pepsin reaching the throat, which gives the alkaline water and the diet more chance to work on what’s already there without constantly being overwhelmed by fresh exposure.
Take it after every meal and before bed for the best effect. The timing matters — taking it before a meal means the food you eat washes it away; taking it after means the raft forms on top of the meal and provides protection during the post-meal window when reflux is most likely to occur.
For the full explanation of how it works, why the UK version specifically matters, and the clinical evidence behind it, see my Gaviscon Advance guide.
Method 5: The Low Acid Diet
The low acid diet addresses pepsin from two angles simultaneously — it reduces the dietary triggers that reactivate dormant pepsin in the throat, and it reduces the overall acid load in the stomach which reduces the frequency and severity of reflux events that send new pepsin upward.
The Zalvan et al. JAMA study (2017) compared a plant-based Mediterranean diet with alkaline water against PPI therapy in 184 LPR patients. The dietary approach — which combined the low acid diet with alkaline water as the main beverage — produced at least equivalent symptom improvement to PPIs, and in some measures outperformed them. 63% of the dietary group achieved a clinically meaningful symptom reduction versus 54% in the PPI group.
This is why diet isn’t optional for LPR. It’s not a lifestyle enhancement — it’s the mechanism by which pepsin reactivation is controlled at the dietary level. The throat spray and alkaline water deal with pepsin in the throat; the diet deals with the conditions that allow that pepsin to keep causing damage.
For a complete structured approach to the diet, check the Wipeout Diet Plan.
What About Future Treatments? The Pepsin Inhibitor Angle
One of the most exciting developments in LPR research is the work being done on fosamprenavir — an existing HIV medication being repurposed as the world’s first specific pepsin inhibitor. Rather than suppressing acid or creating a physical barrier, it blocks pepsin directly at the enzymatic level.
A 2023 study in The Laryngoscope showed fosamprenavir reversed pepsin-induced laryngeal damage in a mouse model of LPR. A Phase II clinical trial is currently underway. This is still some years away from being available as a treatment, but it confirms the research direction — the medical community is increasingly focused on pepsin as the target, not acid.
For now, the combination of alkaline water, alkaline throat spray, low acid diet and Gaviscon Advance gives you the best available tools to manage pepsin without waiting for a pharmacological solution. You can read more about the fosamprenavir research in my dedicated fosamprenavir article.
Putting It All Together
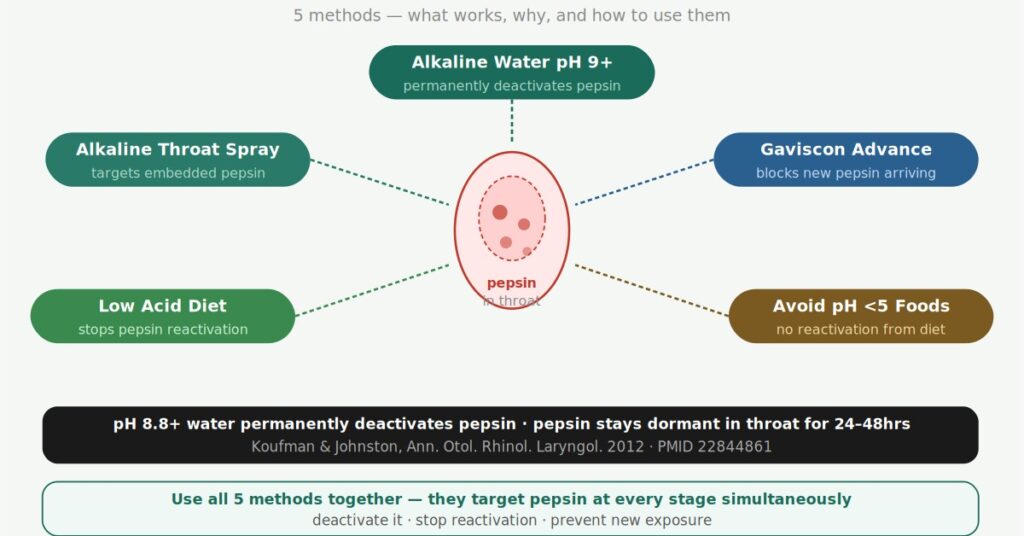
The most effective approach to neutralising pepsin in the throat uses all of these methods together — they work on different parts of the problem simultaneously:
- Alkaline water (pH 9+) as your main drink — permanently deactivates pepsin on contact throughout the day
- Alkaline throat spray — targets pepsin embedded deeper in throat tissue, particularly useful during flare-ups and in early treatment
- Low acid diet (avoid anything below pH 5) — stops dormant pepsin from being reactivated by dietary acids
- Gaviscon Advance after meals and before bed — reduces new pepsin reaching the throat from below
The order in which these matter: diet and Gaviscon Advance first, because without them you’re constantly fighting new pepsin exposure. Alkaline water and throat spray alongside them to deal with what’s already there. Together this is a coherent approach that targets pepsin at every stage — stopping it arriving, deactivating what’s there, and preventing reactivation.
For a personalised plan based on your specific symptoms and situation, consider a private consultation.
Frequently Asked Questions
What permanently deactivates pepsin in the throat?
Alkaline water at pH 8.8 or above permanently and irreversibly deactivates pepsin. This was confirmed by Koufman and Johnston’s 2012 laboratory study published in the Annals of Otology, Rhinology and Laryngology. Once deactivated by sufficiently alkaline water, pepsin cannot be reactivated. Regular water at pH 6.7 to 7.4 has no effect on pepsin at all.
How long does pepsin stay in the throat?
Based on early research, pepsin can remain dormant in throat tissue for up to 24 to 48 hours after a reflux episode. During this window it can be reactivated by anything acidic — food, drink, or another reflux event. This is why consistent use of alkaline water throughout the day is more effective than occasional use.
Does the alkaline throat spray work better than drinking alkaline water?
They serve different purposes. Drinking alkaline water deactivates pepsin in the throat as it passes through and maintains an alkaline environment throughout the day. The throat spray delivers more targeted, sustained contact to the upper throat and voice box where embedded pepsin may be harder to reach with a quick drink. Ideally use both — drinking as your main daily habit, spraying after meals and during flare-ups.
What foods reactivate pepsin in the throat?
Any food or drink with a pH below 5 reactivates dormant pepsin. The main offenders are soft drinks (pH 2.5 to 3.5), coffee (pH 4 to 5), alcohol (pH 3 to 4), citrus fruits and juices (pH 2 to 4), tomatoes and tomato products (pH 3.5 to 4.5), vinegar (pH 2 to 3), and carbonated water (pH 3 to 4). Avoiding these is essential while the throat is healing. See my full LPR foods to avoid guide for the complete list.
Does Gaviscon Advance neutralise pepsin?
No — Gaviscon Advance does not neutralise pepsin directly. What it does is create a physical barrier on top of stomach contents that prevents acid and pepsin from refluxing into the throat. It addresses the source of new pepsin exposure rather than the pepsin already in the throat. That’s why it works best in combination with alkaline water rather than as a standalone treatment.
How quickly will I notice improvement from neutralising pepsin?
Most people who apply the full combination — alkaline water, throat spray, low acid diet and Gaviscon Advance — start to notice improvement within 1 to 2 weeks. Healing of the throat tissue takes longer — typically 4 to 8 weeks for meaningful improvement in throat symptoms and potentially several months for full recovery depending on how long the condition has been active. Consistency is key; sporadic use produces sporadic results.
Conclusion
Pepsin in the throat is the mechanism behind LPR symptoms, and neutralising it is the central goal of effective LPR management. Alkaline water at pH 8.8 or above permanently deactivates it. The alkaline throat spray delivers this more directly to embedded pepsin in throat tissue. The low acid diet stops reactivation. Gaviscon Advance reduces new pepsin exposure. Used together these methods give you a comprehensive approach that targets pepsin at every stage of the problem.
Related articles:
- The Complete Guide to LPR — Causes, Symptoms and Treatment
- Alkaline Water for LPR — What pH You Need and Why
- Gaviscon Advance for LPR — Why It Works and How to Use It
- LPR Foods to Avoid — The Complete List
- LPR Diet — What to Eat and What to Avoid
- Silent Reflux Treatment — What Actually Works
- Fosamprenavir for LPR — The New Pepsin Inhibitor in Development
References
- Koufman JA, Johnston N. (2012) “Potential benefits of pH 8.8 alkaline drinking water as an adjunct in the treatment of reflux disease.” Annals of Otology, Rhinology and Laryngology, 121(7):431-434. PubMed PMID 22844861
- Johnston N, Dettmar PW, Bishwokarma B, Lively MO, Koufman JA. (2007) “Activity/stability of human pepsin: implications for reflux attributed laryngeal disease.” The Laryngoscope, 117(6):1036-9. PubMed PMID 17417109
- Zalvan CH et al. (2017) “A Comparison of Alkaline Water and Mediterranean Diet vs Proton Pump Inhibition for Treatment of Laryngopharyngeal Reflux.” JAMA Otolaryngology-Head and Neck Surgery, 143(10):1023-1029. PMC5710251
- Johnston N, Samuels TL, Goetz CJ, et al. (2022) “Oral and Inhaled Fosamprenavir Reverses Pepsin-Induced Damage in a Laryngopharyngeal Reflux Mouse Model.” The Laryngoscope. PubMed PMID 35678265
David Gray
Content Researcher & Author
David Gray founded Wipeout Reflux to address a critical gap in reflux management. His research synthesizes over 100 peer-reviewed studies on laryngopharyngeal reflux (LPR), pepsin biology, and GERD pathophysiology. For LPR specifically—a condition most physicians misdiagnose—his work focuses on pepsin reactivation and why standard PPI therapy fails most patients. He develops evidence-based protocols targeting root causes of both LPR and GERD, integrating emerging research on sphincter dysfunction, dietary interventions, and newer clinical approaches. Wipeout Reflux represents practical application of clinical science for patients seeking real solutions.

Happy to find your website! YEARS of heartburn.. dr just gave to me a scrip for a PPI which I didn’t pick up. I have been using baking soda and water (2-4x per day). I know the side effects of ppi..All docs do that. I’m not happy just treating with those side effects. So i’m here to find another strategy. Now I need to find those little spray bottles. I think my nasal spray bottles will work fine. I’m so grateful you explained the pepsin issue. Never heard that before. But I am changing my diet to more alkaline and less acid.
But I’m curious about the melatonin. And my husband would love to know if my snoring will ease up—on his ears!😅
Great that you didn’t just blindly jump on a PPI — most doctors hand them out like sweets without ever explaining *why* you’re refluxing in the first place.
Baking soda can give quick relief, but 2–4x per day long-term isn’t ideal (it’s a lot of sodium and it can cause rebound issues). The spray bottle idea is fine — a clean nasal spray bottle usually works perfectly as long as it produces a light mist.
On melatonin: it’s interesting because it’s not just a “sleep supplement”. Some studies suggest it may help reflux by improving LES tone and reducing irritation. Most people start low (like **1mg**) and see how they respond. No need to mega-dose it.
And yes — if your reflux/LPR is contributing to throat swelling and nasal congestion, snoring often improves as the inflammation settles down. Your husband may actually become a fan of the alkaline diet too 😄
Hi David…how can I reach the vocal cords with a sprayer?
You realistically **can’t directly spray your vocal cords** (and you shouldn’t try to force it).
The goal of the spray isn’t to perfectly “hit” the cords — it’s to **coat the throat area** where pepsin sits and where irritation is happening. If you spray the back of the throat and upper airway, you’re still doing what matters.
What usually works best is:
* spray toward the **back of the throat** (mouth open, aim slightly downward)
* do a couple of sprays
* then **swallow gently** so it coats deeper tissues
Even if it doesn’t feel like it’s reaching the cords, it still helps because the irritated area is generally the whole throat/larynx region, not just the cords themselves.
Hello,
I am very pleased to read your posts on LPR.
Gargling with low pH water and spraying the throat are excellent help.
I am curious as to how the melatonin may assist please?
Strangely I seem to be atypical in as much as when I lie down I have no irritation of the throat at all which afford me rest, however I work standing up and need to talk all day.
Any advice would be greatly appreciated,
Kind regards
Hello, and thank you for the kind words.
Some research suggests melatonin may help reflux by supporting LES function, digestion, sleep quality, and reducing irritation/inflammation, although the evidence is still fairly limited overall. Some people with LPR seem to benefit from it, especially with nighttime symptoms, while others notice little difference.
And you’re actually not alone in being more symptomatic upright rather than lying down. LPR can present very differently between people, and prolonged talking/standing during the day can sometimes aggravate throat irritation and vocal strain significantly.
Hopefully continuing to reduce irritation and giving the throat time to calm down helps things improve gradually.
Hello David,
Your web site is very interesting. Just diagnosed with LPR although I must have had it for over a year. All the usual symptoms. Was prescribed PPI’s but learned they are not effective for LPR. There are a lot of different ideas about how to ease the symptoms of LPR but apart from diet (which does not apply in my case) there was little talk about the cause. I was happy to read your comments about the lower esophageal sphincter as I believe that is where the problem lies. I have just started Melatonin and I also gargle with alkaline water with added bi-carb. Thanks for your article, haven’t read it all yet.
Sandra (Australia)
Hi Sandra,
Yes I totally agree wiht you, some things that work for some dont work at all for others and vice versa. Oh great, melatonin is a great choice. Did it help you?
Hi,
I am also having LPR for past 4 years but diagnosis was confirmed only recently. How did the Melatonin supplement help? How long before it shows LES tightening? Thanks!
Mugundhan
Hi Mugundhan,
Some studies and anecdotal reports suggest melatonin may help reflux by supporting LES tone, digestion, and reducing irritation/inflammation, although the research is still fairly limited overall. Some people with LPR notice improvement in sleep and nighttime reflux symptoms from it, while others notice little difference.
If it does help, it’s usually something people notice gradually over a few weeks rather than immediately “tightening” the LES overnight. Also, not everyone tolerates melatonin the same way, so it’s generally best to start with a low dose.
I’d still view it more as a supportive tool alongside diet and lifestyle changes rather than a standalone fix for LPR.