If you have symptoms of LPR or silent reflux and you’ve been trying to figure out whether reflux is actually the cause, you may have come across the Peptest. It’s a saliva test you can do at home that detects pepsin — the digestive enzyme at the root of most LPR symptoms — and it’s become increasingly popular as a way to get some kind of diagnostic confirmation without going through expensive or invasive medical testing.
In this article I’m going to give you an honest, balanced assessment of what the Peptest is, how it works, what the research actually shows about its accuracy, and whether it’s worth doing in your situation. I’ll be straight about both the strengths and the limitations — because there’s a bit of nuance here that most articles on the topic skip over.
Key Takeaways:
- Peptest detects pepsin in saliva — a positive result is a strong indicator of LPR, with a specificity of around 74–100% depending on the study
- Sensitivity is moderate — a negative result doesn’t rule out LPR, as the test misses around 30–40% of confirmed LPR cases
- A positive Peptest result is more useful than a negative one — if you test positive, that’s meaningful
- Multiple samples taken at different times of day improve accuracy significantly
- It’s useful as a first-line supportive tool but is not a replacement for clinical assessment or 24-hour pH impedance monitoring
- The RSI test is a free, reliable first step for self-assessment — Peptest adds value on top of this but doesn’t replace it
What Is Peptest?
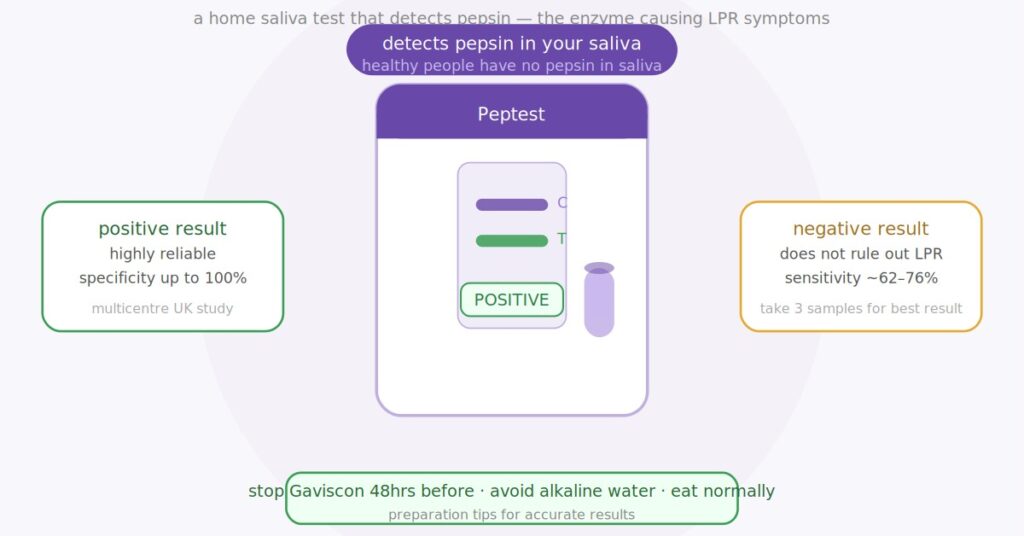
Peptest is a rapid lateral flow test manufactured by RD Biomed (based in Hull, UK) that detects the presence of pepsin in your saliva. It works in a similar way to a pregnancy test or a COVID lateral flow test — you add a saliva sample to a tube containing a citric acid solution, apply it to the test strip, and the result shows within minutes.
The logic behind it is straightforward. Pepsin is a digestive enzyme produced in the stomach. In a healthy person with no reflux, pepsin stays in the stomach where it belongs and should not be detectable in saliva. If you have LPR, pepsin travels up through the oesophagus and into the throat and mouth during reflux episodes — and this is what the test is detecting. Finding pepsin in your saliva is a sign that you’ve been refluxing into your throat.
The test comes as a kit that you order online, do at home, and then either send back to the lab for professional analysis or read yourself using the test strips. Depending on the version you order you’ll typically provide three saliva samples — one on waking, one an hour after a meal, and one at another point during the day. The concentration of pepsin detected (measured in nanograms per millilitre) is then reported in your results.
How Accurate Is Peptest for LPR?
This is the honest part — and it’s important to understand before deciding whether to spend money on the test.
The research on Peptest accuracy shows a consistent pattern across multiple studies: good specificity but moderate sensitivity. In plain terms, that means a positive result is fairly reliable, but a negative result doesn’t necessarily mean you don’t have LPR.
Here’s what the key studies show:
A systematic review and meta-analysis (Guo et al., 2021) covering 16 studies with 2,401 patients and 897 controls found pooled sensitivity of 62% and specificity of 74% for Peptest across LPR and GERD diagnoses. In other words — the test correctly identifies around 62% of people who actually have LPR, and correctly clears around 74% of people who don’t.
A large multicentre UK study across five voice clinics with over 1,000 LPR patients reported better results — sensitivity of 76.4% and specificity of 100%. The 100% specificity is significant: in this study, if the test came back positive, every single positive result was a true positive. No healthy person in the control group had a positive pepsin result.
A 2024 prospective cohort study (Lechien et al.) looking specifically at fasting and bedtime sample timing found that using both samples together and taking the highest reading improved sensitivity to 81.6% — considerably better than a single sample. The positive predictive value (PPV) at this point was 93%, meaning if you test positive with this protocol, there’s a 93% chance you genuinely have LPR.
A 2023 study by Lechien et al. was more cautious — it found Peptest was not reliable for detecting GERD in LPR patients specifically, and concluded that consistency between Peptest results and gold-standard pH impedance monitoring was not significant. This is an important caveat.
The bottom line from the research: a positive Peptest result is meaningful and worth taking seriously. A negative result should not be used to rule out LPR.
Peptest vs Other LPR Diagnostic Methods
To put Peptest in context it helps to know what the alternatives are — because LPR is notoriously difficult to diagnose reliably and none of the options are perfect.
| Method | Invasive? | Cost | Accuracy | What it shows |
|---|---|---|---|---|
| RSI test | No | Free | Good for symptom assessment | Symptom severity score |
| Peptest | No | ~£60–£100 | Moderate (62–84% sensitivity, 74–100% specificity) | Presence and concentration of pepsin in saliva |
| Laryngoscopy | Mildly | NHS or private consult | Good for visible signs — not specific to LPR | Inflammation, redness, granulation in throat |
| 24hr pH impedance (HEMII-pH) | Yes | £500–£2,000+ | Gold standard | Number, type and timing of reflux events |
| Restech pH study | Mildly | Private only | Good for pharyngeal pH | Acid levels in the throat specifically |
Peptest sits usefully between the free symptom-based RSI test and the expensive, invasive gold-standard 24-hour pH impedance monitoring. For most people it’s a reasonable middle ground — more objective than a symptom score, far cheaper and less invasive than hospital-based testing.
For more on the RSI test check my article on the RSI test for LPR. For more on Restech check my article on Restech pH monitoring.
How to Do Peptest — Step by Step
The test itself is genuinely simple. Here’s how it works:
1. Order the kit — Peptest is available directly from peptest.co.uk (UK and worldwide) or via The Reflux Company in the US. The standard kit comes with collection tubes and prepaid return packaging for lab analysis.
2. Collect saliva samples at the right times — the standard protocol involves three samples:
- Sample 1: first thing in the morning, before eating or drinking anything
- Sample 2: one hour after your main meal
- Sample 3: at another point in the day, ideally when you feel symptoms
3. Add saliva to the tube — each tube contains citric acid which preserves pepsin activity. You spit into the tube, seal it, and store it refrigerated until you’re ready to send.
4. Return the samples — send the sealed tubes back to the lab using the prepaid packaging included in the kit. Results are typically returned within a few days.
5. Read your results — results show whether pepsin was detected and at what concentration (in ng/mL). A reading above 16 ng/mL is generally considered a positive result, though some studies suggest higher thresholds of 75 ng/mL give better specificity.
A few important things to know before you test:
- Do not take Gaviscon Advance, alginate suspensions or antacids for 48 hours before and during the test period — these can affect pepsin levels in saliva
- PPIs and other prescription medications can generally be continued during the test
- Eat your normal diet during the test day — the point is to capture what your reflux actually looks like, not an artificially clean day
- Alkaline water should be avoided during the test period as it deactivates pepsin and will produce a false negative
What Do Your Peptest Results Mean?
Positive result
A positive result — pepsin detected at 16 ng/mL or above — is a meaningful finding. It means pepsin from your stomach has reached your saliva which is not something that happens in healthy people without reflux. Based on the multicentre UK study, a positive result has a specificity of up to 100%, meaning if you test positive it’s very likely you are genuinely refluxing into the throat.
The higher the concentration of pepsin detected, the more significant the reflux is likely to be. A positive Peptest result is a good reason to take the diagnosis seriously and start the appropriate treatment — the low acid diet, Gaviscon Advance (UK version) and the lifestyle changes covered in my silent reflux treatment guide.
Negative result
A negative result is more complicated and requires careful interpretation. Because sensitivity is moderate — around 62 to 84% depending on the protocol — a negative result does not mean you don’t have LPR. The test may have missed a positive because:
- You didn’t reflux during the sampling window — LPR reflux is intermittent, not constant
- You only provided one or two samples — more samples at different times significantly improve the detection rate
- Your reflux is predominantly weakly acidic or non-acidic — some forms of LPR involve less acid which affects pepsin activity and detection
As a 2023 study (Lechien et al.) concluded: collecting multiple saliva samples improves detection rate considerably, and in cases of high clinical suspicion and a negative pepsin result, 24-hour pH impedance monitoring is the next appropriate step.
In short — if you test negative but still have significant symptoms matching LPR, take the RSI test and consider speaking to a specialist rather than treating the negative result as definitive.
Is Peptest Worth Doing?
My honest view is that Peptest is a useful tool in certain situations but it’s not essential for everyone — and it needs to be understood properly to be used well.
It’s worth doing if:
- You want objective evidence of pepsin in your throat before committing to a significant dietary change
- You’ve had a negative 24-hour pH test but still strongly suspect LPR — a positive Peptest adds a different data point
- You want to monitor whether treatment is working — a follow-up test can show whether pepsin concentrations have reduced
- You need documentation to support a referral to a specialist
It’s probably not essential if:
- You score highly on the RSI test and your symptoms clearly point to LPR — at that point starting the right treatment is more useful than waiting for a test result
- You’ve already had a formal diagnosis from an ENT or gastroenterologist
- Cost is a concern — the RSI test is free and a good starting point
The most important thing is to not let the Peptest replace clinical judgement. A negative Peptest in someone with a high RSI score and classic LPR symptoms should not stop you from starting treatment. And a positive Peptest doesn’t mean you can skip the diet and lifestyle changes in favour of medication alone.
If you want guidance on your specific situation — including what tests might be worth doing and what treatment approach makes most sense for you — that’s exactly what a private consultation is for.
Frequently Asked Questions
What does Peptest actually test for?
Peptest detects the presence of pepsin in your saliva. Pepsin is a digestive enzyme produced in the stomach. In healthy people it stays in the stomach — finding it in saliva indicates it has travelled up through the oesophagus into the throat and mouth during reflux episodes. This makes it a useful biomarker for LPR specifically.
Can Peptest diagnose LPR on its own?
Not definitively on its own. A positive Peptest result strongly supports an LPR diagnosis and is very unlikely to be a false positive. A negative result, however, does not rule out LPR — the test misses around 20 to 40% of confirmed LPR cases depending on how many samples are taken and when. It should be used alongside clinical assessment and the RSI test rather than as a standalone diagnostic tool.
How accurate is Peptest?
Across multiple studies and a meta-analysis covering 2,400+ patients, Peptest has a pooled sensitivity of around 62–76% and specificity of 74–100% for LPR. Sensitivity improves significantly when multiple samples are taken at different times of day — using three samples (morning, post-meal, and evening) gives the most reliable result. A positive result is particularly meaningful given the high specificity reported in the largest multicentre study.
How long does Peptest take?
Collecting your samples takes a few minutes spread across one day. Once you send the samples back to the lab, results are typically returned within 2 to 5 working days.
Can I do Peptest while taking Gaviscon Advance?
No — you need to stop taking Gaviscon Advance and other alginate-based products for at least 48 hours before and during your test period. Alginates bind to pepsin and remove it from the refluxate, which will produce artificially low pepsin readings. PPIs and other prescription medications are generally fine to continue during the test.
Should I avoid alkaline water before Peptest?
Yes — alkaline water with a pH above 8 permanently deactivates pepsin, so drinking it before or during the test will give you a false negative. Stick to regular still water during the test period.
Is Peptest available in the US?
Yes — in the US it’s available as PepsinCheck through The Reflux Company. The test is identical to the UK version — it’s the same product manufactured by RD Biomed, just distributed differently. Check refluxcompany.com for the US version.
What should I do after a positive Peptest result?
A positive result confirms pepsin is reaching your throat and is a good reason to start treatment seriously. The core approach is a strict low acid diet — avoiding foods and drinks with a pH below 5 — alongside Gaviscon Advance (UK version) after meals and before bed. Check my complete LPR treatment guide for the full approach.
Conclusion
Peptest is a genuinely useful non-invasive tool for supporting an LPR diagnosis — particularly because a positive result is so specific that it’s hard to argue with. The limitation is on the sensitivity side: a negative result doesn’t clear you, especially if your symptoms are clearly pointing to LPR.
My recommendation is to use it as one piece of the puzzle alongside the RSI test rather than as the sole basis for your decision. If you test positive, start treatment. If you test negative but still have significant symptoms, don’t take it as a definitive all-clear — consider further testing or a consultation.
For more on how LPR is diagnosed and what the next steps look like check my complete guide to LPR. And for a structured treatment plan check the Wipeout Diet Plan.
Related articles:
- RSI Test — Do You Have LPR?
- Restech pH Monitoring for LPR
- The Complete Guide to LPR — Causes, Symptoms and Treatment
- LPR Symptoms — The Complete Guide
- Silent Reflux Treatment — What Actually Works
- Gaviscon Advance for LPR
- LPR Diet — What to Eat, What to Avoid and What to Drink
- GERD vs LPR — What’s the Difference?
References
- Guo Z et al. (2021) “Salivary peptest for laryngopharyngeal reflux and gastroesophageal reflux disease: A systematic review and meta-analysis.” Medicine, 100(32):e26756. PMC
- Dettmar PW et al. (2019) “A Multicentre Study in UK Voice Clinics Evaluating the Non-invasive Reflux Diagnostic Peptest in LPR Patients.” SN Comprehensive Clinical Medicine. Full text
- Lechien JR et al. (2024) “Diagnostic Value of Fasting and Bedtime Saliva Pepsin Measurements in Laryngopharyngeal Reflux.” Diagnostics. PMC
- Lechien JR, Bobin F. (2023) “Saliva pepsin measurements in the detection of gastroesophageal reflux disease in laryngopharyngeal reflux patients: a cohort study.” European Archives of Oto-Rhino-Laryngology, 280(8):3765-3771. PubMed
- Lechien JR et al. (2023) “Variability and accuracy of multiple saliva pepsin measurements in laryngopharyngeal reflux patients.” Journal of Otolaryngology — Head and Neck Surgery, 52(1):66. PubMed
- Zhang M et al. (2021) “Diagnostic Utility of Salivary Pepsin as Compared With 24-Hour Dual pH/Impedance Probe in Laryngopharyngeal Reflux.” Otolaryngology — Head and Neck Surgery, 164(2):375-380. PubMed
- Wang L et al. (2017) “Pepsin in saliva as a diagnostic biomarker in laryngopharyngeal reflux: a meta-analysis.” European Archives of Oto-Rhino-Laryngology. PubMed
- NICE. (2015) “Peptest for diagnosing gastro-oesophageal reflux: Evidence review.” NICE
David Gray
Content Researcher & Author
David Gray founded Wipeout Reflux to address a critical gap in reflux management. His research synthesizes over 100 peer-reviewed studies on laryngopharyngeal reflux (LPR), pepsin biology, and GERD pathophysiology. For LPR specifically—a condition most physicians misdiagnose—his work focuses on pepsin reactivation and why standard PPI therapy fails most patients. He develops evidence-based protocols targeting root causes of both LPR and GERD, integrating emerging research on sphincter dysfunction, dietary interventions, and newer clinical approaches. Wipeout Reflux represents practical application of clinical science for patients seeking real solutions.