Yes — silent reflux can be cured. I know because I did it myself after three years of symptoms, misdiagnoses, and treatments that made no difference. On this page I am going to walk you through exactly what I did to recover, why each step works, and what the clinical research says to back it up.
This is not generic advice. This is the specific approach that worked for me and has since helped hundreds of people who have come to me through consultations and this site. Most people who follow this correctly start seeing improvement within one to two weeks.
Key Takeaways:
- Silent reflux (LPR) can be cured or significantly improved in the majority of cases
- The two most important steps are a strict low acid diet and Gaviscon Advance (UK version) after meals
- PPIs are the most commonly prescribed treatment for LPR and have been proven in clinical trials to be no better than placebo — stopping them (slowly) is often part of recovery
- A 2025 prospective clinical study confirmed that diet and lifestyle changes alone significantly reduced LPR symptoms and physical findings
- Most people see meaningful improvement within 1–2 weeks of following the right approach consistently
- Full recovery typically takes 2–6 months depending on severity
My Story — Three Years of Getting It Wrong Before Getting It Right
I developed LPR (Laryngopharyngeal Reflux) without knowing what it was. The sore throat that never went away. The constant need to clear my throat. The hoarseness. The feeling of something stuck. I went to my GP, was referred to a specialist, had tests — and came away with PPIs and very little else.
The PPIs did nothing. The symptoms kept building. I tried different medications, different supplements, different approaches — most of which made no difference and some of which made things worse. What frustrated me most wasn’t the discomfort. It was the total absence of useful information. Nobody I saw seemed to understand what LPR actually was or how it actually needed to be treated.
So I started researching everything I could find. I read the clinical studies, traced the research back to primary sources, and slowly built a picture of what was actually happening and what would actually help. I implemented the approach I am going to describe below. Within two weeks I noticed a clear improvement. Within six months I was fully recovered.
That was eight years ago. I have not had a significant LPR flare since.
Why Most LPR Treatment Fails — The PPI Problem
Before covering what works it is important to understand why what most people are given does not work — because this is the reason so many people are stuck.
The standard medical response to LPR is to prescribe PPIs (proton pump inhibitors like omeprazole or lansoprazole). These drugs reduce stomach acid production. For regular acid reflux and GERD they can be effective. For LPR they are not — and the research is definitive on this point.
The reason PPIs fail for LPR is that the primary driver of LPR symptoms is not acid — it is pepsin, a digestive enzyme that travels up from the stomach into the throat during reflux episodes. Pepsin causes direct tissue damage and inflammation in the throat even in weakly acidic or non-acidic conditions. Reducing stomach acid with PPIs does not stop pepsin from causing damage. It addresses the wrong thing entirely.
The TOPPITS randomised controlled trial published in the BMJ (O’Hara et al., 2021) — the largest study of its kind — confirmed that PPIs were no better than placebo for persistent throat symptoms. The 2024 IFOS international consensus now formally states that acid suppression should not be considered first-line therapy for isolated LPR symptoms.
If you are currently on PPIs and they are not helping, this is exactly why. And if you want to stop them, you cannot do it suddenly — there is a severe rebound acid effect. Read my guide on getting off PPIs safely before you stop.
How I Cured My Silent Reflux — The Exact Steps
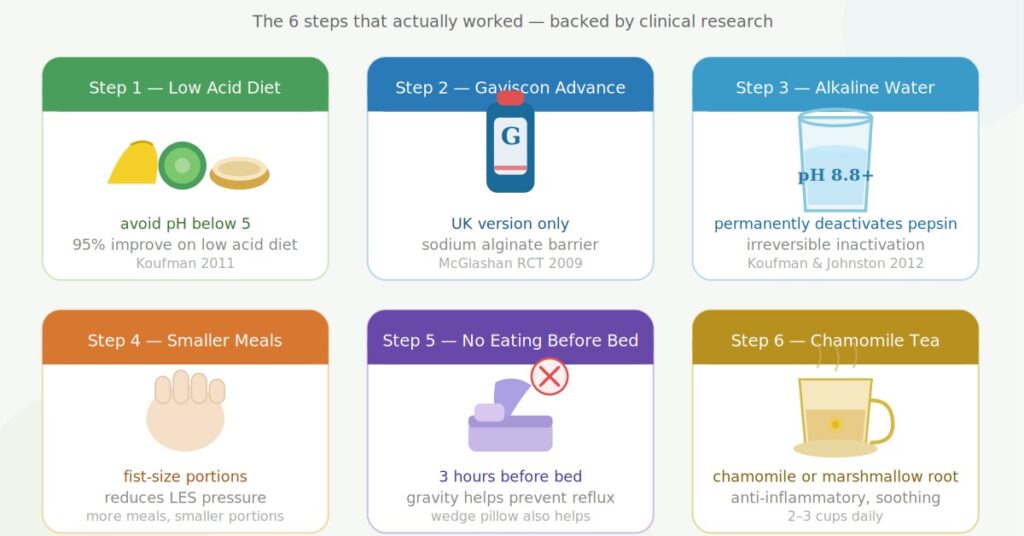
These are the six things that made the difference for me, in order of importance. I am not going to bury the most important ones at the bottom — the diet and Gaviscon Advance are what actually moved the needle. Everything else is supportive.
Step 1: The Low Acid Diet — The Single Most Important Thing

The low acid diet is the most powerful treatment available for LPR. I cannot overstate how much of a difference this made for me — within a week of following it strictly my symptoms started to noticeably reduce for the first time in years.
The diet works because of how pepsin behaves. After a reflux episode, pepsin deposits itself in the cells of the throat where it can sit dormant for 24 to 48 hours. If you eat or drink anything with a pH of 5 or below during that time, the pepsin gets reactivated and your symptoms flare — even if you haven’t refluxed again. The diet breaks this cycle by keeping the pH of your food and drink above 5, preventing reactivation and giving your throat the opportunity to heal.
The clinical evidence for this is strong. A prospective study by Dr Jamie Koufman found that 95% of LPR patients improved on a strict low acid diet — including patients who had already failed twice-daily PPI treatment. A cross-over study published in The Laryngoscope (Lechien et al., 2022) confirmed a low-fat, high-protein, alkaline, plant-based diet was an effective standalone treatment for LPR. And a 2025 prospective study (Lechien et al.) confirmed that diet and lifestyle changes alone significantly reduced both LPR symptoms and objective laryngeal findings over 6 to 12 weeks.
A 2025 systematic review of diet recommendations for LPR covering 868 patients found that diet adherence led to significant symptom reduction in 54% to 83% of untreated patients — comparable to medication effectiveness.
What I cut out completely
- All soft drinks, carbonated drinks, fruit juice and alcohol — these are some of the most acidic things you can consume
- Coffee — even decaf is acidic enough to reactivate pepsin
- All citrus fruits and juices
- Tomatoes and tomato-based products
- Spicy food
- Fatty and fried foods — these slow gastric emptying and worsen reflux
- Chocolate
- Processed foods
- Mint
What I ate instead
Oats, rice, lean chicken and fish, most vegetables (particularly cucumber, celery, broccoli and courgette), bananas, melon, watermelon, almonds, chamomile tea and alkaline water. Simple, whole food, low acid eating.
For a complete food and drink guide check my LPR diet article, my foods to eat guide and my foods to avoid guide. If you want a fully structured plan with everything laid out check the Wipeout Diet Plan — I created it specifically for people with LPR and GERD based on the same approach that healed me.
Step 2: Gaviscon Advance (UK Version) — The Right Medication
Gaviscon Advance (UK version) was the only medication that made a genuine difference for me and it is the one I recommend to everyone with LPR. It works completely differently to PPIs. Rather than reducing stomach acid it creates a physical alginate raft on top of the stomach contents that acts as a barrier, preventing reflux from reaching the throat and filtering pepsin before it can do damage.
The key ingredient is sodium alginate — derived from seaweed — which forms this protective raft when it hits stomach acid. It also helps neutralise and remove any pepsin already present in the throat, actively working to reduce existing damage rather than just preventing new damage.
The clinical evidence is solid. A randomised controlled trial by McGlashan et al. found Gaviscon Advance produced significant improvements in LPR symptom scores at both 2 and 6 months compared to no treatment. A study by Wilkie et al. (2018) found Gaviscon Advance alone was effective for LPR and that adding a PPI on top of it provided no additional benefit whatsoever.
The most important thing: you must use the UK version. The US version of Gaviscon has completely different ingredients and does not contain sodium alginate. It will not work for LPR. The UK version is available on Amazon here if you are outside the UK.
Take it 15 to 30 minutes after every meal and before bed. For everything you need to know about it check my article on Gaviscon Advance for LPR.
Step 3: Alkaline Water
Drinking alkaline water with a pH of 8 or above was something I added after reading the research and it made a noticeable difference, particularly in the mornings when symptoms were often at their worst.
A study by Koufman and Johnston published in the Annals of Otology, Rhinology and Laryngology (2012) found that water with a pH of 8.8 permanently deactivates pepsin — not just suppresses it, but destroys it. Regular tap and bottled water (typically pH 6.7 to 7.4) has no effect on pepsin. Alkaline water above pH 8.8 irreversibly inactivates it.
Aim to drink alkaline water throughout the day — particularly first thing in the morning, after meals and whenever you feel symptoms flaring. For more detail check my article on alkaline water for LPR.
Step 4: Smaller Meals More Frequently
This was one of those changes I underestimated at first but it made a bigger difference than I expected. Large meals overfill the stomach and put excessive pressure on the lower oesophageal sphincter (LES) — the valve above the stomach that is supposed to keep everything in place. When the stomach is overloaded the LES cannot maintain its seal and reflux occurs much more easily.
The fix is simple: eat roughly a fist-sized portion at any one sitting and spread your food intake across more meals throughout the day rather than two or three large ones. You are not eating less overall — just distributing it differently. For more on how the sphincter works check my article on the stomach sphincter’s role in LPR.
Step 5: No Eating Within 3 Hours of Bedtime
This was non-negotiable for my recovery. When you lie down, gravity no longer helps keep stomach contents in place. If you have eaten recently, the risk of reflux is dramatically increased — and nighttime reflux is particularly damaging because the pepsin sits in your throat for hours without being cleared.
I set a hard rule: nothing to eat or drink other than water after 7pm. It was difficult for the first week and became automatic after that. Alongside this I used a wedge pillow to elevate my head by around 6 to 8 inches which uses gravity to further reduce nighttime reflux. For more advice on this check my article on acid reflux at night.
Step 6: Chamomile and Marshmallow Root Tea
I tried many things to soothe my throat symptoms while healing — lozenges, throat sprays, various supplements. Most made no meaningful difference and some irritated things further. The two things that genuinely helped were chamomile tea and marshmallow root tea.
Chamomile is anti-inflammatory, naturally alkaline and genuinely soothing on inflamed throat tissue. I drank two to three cups a day throughout recovery. Marshmallow root creates a mucilaginous coating on the throat that helps protect and soothe irritated tissue. Both are excellent drink alternatives to water for people with LPR. For more on this check my article on chamomile tea and acid reflux.
How Long Does It Take to Cure Silent Reflux?
Most people following this approach notice meaningful improvement within 1 to 2 weeks. That does not mean full recovery — it means a clear and noticeable reduction in symptoms that tells you the approach is working.
Full recovery typically takes 2 to 6 months depending on how long you have had LPR and how severe it has been. For me it took 6 months to be completely symptom-free, but I had been symptomatic for several years and was in a fairly advanced state. People who catch it earlier tend to heal faster.
The physical healing of laryngeal tissue — the redness, swelling and granulation that an ENT can see on laryngoscopy — lags behind how you feel. Your symptoms will improve before the visible signs resolve. Research supports continuing the treatment approach for at least 6 months to allow full resolution of physical findings even if you feel significantly better before then.
The most important factor is consistency. One or two days of eating acidic food or drinking coffee can set you back noticeably because of how pepsin reactivation works. The stricter you are in the first 6 to 8 weeks, the faster you will heal.
Can Silent Reflux Come Back After Being Cured?
Yes it can — if you go back to the diet and lifestyle that triggered it in the first place. For me, returning to drinking alcohol and coffee regularly would almost certainly bring symptoms back. Most people who have had LPR find they have a lower threshold for trigger foods than they did before, and need to be mindful of this long term.
That said, the majority of people do not need to follow the strict acute-phase diet permanently. Once fully healed most people can reintroduce a wider range of foods and drinks while keeping the obvious high-acidity triggers in check. It is about finding your personal threshold rather than following the acute diet indefinitely.
What If the Diet and Gaviscon Aren’t Working?
If you have followed the diet strictly for 3 to 4 weeks and taken Gaviscon Advance after every meal and still see no improvement, the most likely reasons are:
- You are still consuming something acidic without realising it — coffee, certain herbal teas, fizzy water, most condiments and many processed foods are all acidic enough to reactivate pepsin
- You have an underlying issue driving the LPR — SIBO (small intestinal bacterial overgrowth) is a surprisingly common root cause that doesn’t respond to dietary changes alone until it is addressed
- You need more targeted guidance based on your specific situation
If you want personalised help figuring out what is going on and what needs to change, a private consultation is the most direct way to get there. I’ll go through your symptoms, your diet, what you have tried and what the right next steps are for your situation specifically. 86% of people who follow the recommendations from a consultation see meaningful improvement within two weeks.
Frequently Asked Questions
Can silent reflux be cured permanently?
Yes — for the majority of people silent reflux can be fully resolved with the right approach. A strict low acid diet combined with Gaviscon Advance (UK version) is the core treatment. Most people achieve full recovery within 2 to 6 months. Some people need to maintain dietary changes long term to prevent recurrence, but the acute symptoms resolve completely for most who follow the approach consistently.
How do you cure LPR naturally without medication?
The most effective natural treatments for LPR are a strict low acid diet avoiding foods and drinks with a pH below 5, alkaline water with a pH of 8 or above (which permanently deactivates pepsin), eating smaller portions, not eating within 3 hours of bedtime, and chamomile or marshmallow root tea. A 2025 clinical study confirmed diet and lifestyle changes alone significantly reduced LPR symptoms without medication.
How long does LPR take to heal?
Most people following the correct treatment approach notice improvement within 1 to 2 weeks. Full healing typically takes 2 to 6 months depending on severity and how long the condition has been present. Laryngeal tissue damage visible on laryngoscopy takes longer to resolve than subjective symptoms. Consistency with the diet is the biggest determinant of how quickly you heal.
What is the fastest way to cure LPR?
The fastest path to LPR recovery is to combine all of the steps simultaneously from day one: strict low acid diet, Gaviscon Advance (UK version) after every meal, alkaline water throughout the day, smaller meals, no eating within 3 hours of bedtime and stopping PPIs slowly if you are currently on them. Doing all of these consistently from the start gives the best chance of rapid improvement. Most people who are strict with all of these report noticeable improvement within 7 to 14 days.
Is LPR curable or just manageable?
For most people LPR is fully curable rather than just manageable. The distinction matters — management implies permanent ongoing treatment, whereas cure means the underlying condition resolves and you return to normal function. The majority of people who follow the right treatment approach do not need to remain on ongoing treatment indefinitely. Some need long-term dietary adjustments, but the active symptomatic phase resolves completely.
Can stress cause silent reflux to come back?
Yes — stress and anxiety directly worsen LPR through multiple mechanisms. Stress increases gastric acid production, affects gut motility, and lowers the threshold at which the LES relaxes inappropriately. Research has confirmed that anxiety and stress levels are significantly higher in LPR patients and that psychological stress directly impacts symptom severity. If you are going through a stressful period you may notice a flare even while following the diet well. For more on this check my article on LPR and anxiety.
What should I do first if I think I have LPR?
Take the RSI (Reflux Symptom Index) test — it is the most reliable self-assessment tool for LPR and takes two minutes. If your score suggests LPR, read my silent reflux treatment guide and LPR diet guide and start the low acid diet and Gaviscon Advance immediately. The sooner you start the right approach the faster you will recover.
Conclusion
Silent reflux can be cured. I know this from personal experience — and from watching hundreds of people go through the same process I did and come out the other side.
The approach that works is not complicated: a strict low acid diet that keeps food and drink above pH 5, Gaviscon Advance (UK version) after every meal, alkaline water, smaller portions, no eating before bed and stopping the PPIs that are making no difference. Done consistently over 2 to 6 months this resolves LPR for the vast majority of people.
The Wipeout Diet Plan covers the diet side of this in complete detail — everything you need to know about what to eat, what to avoid, what to drink, and how to structure your meals. You can check it out here: Wipeout Diet Plan.
And if you want personalised guidance on your specific situation — particularly if you have been struggling for a while without improvement — a private consultation is the most direct route to answers.
You can get better. The right information and the right approach make all the difference.
Related articles:
- The Complete Guide to LPR — Causes, Symptoms and Treatment
- Silent Reflux Treatment — What Actually Works
- LPR Diet — What to Eat, What to Avoid and What to Drink
- LPR Symptoms — The Complete Guide
- Gaviscon Advance for LPR — Why the UK Version Matters
- Alkaline Water for LPR
- Getting Off PPIs Safely
- RSI Test — Do You Have LPR?
- LPR Foods to Avoid
- Acid Reflux at Night
References
- Koufman JA. (2011) “Low-acid diet for recalcitrant laryngopharyngeal reflux: therapeutic benefits and their implications.” Annals of Otology, Rhinology and Laryngology, 120(5):281-287. PubMed
- O’Hara J et al. (2021) “Use of proton pump inhibitors to treat persistent throat symptoms: multicentre, double blind, randomised, placebo-controlled trial.” BMJ, 372:m4903. BMJ
- Lechien JR et al. (2024) “The Dubai definition and diagnostic criteria of laryngopharyngeal reflux: the IFOS consensus.” The Laryngoscope, 134(4):1614-1624. PubMed
- Lechien JR et al. (2022) “Is Diet Sufficient as Laryngopharyngeal Reflux Treatment?” The Laryngoscope, 132:1916-1923. PubMed
- Lechien JR et al. (2025) “Effectiveness of Diet and Lifestyle Changes for the Treatment of Laryngopharyngeal Reflux Disease.” Journal of Voice. PubMed
- Gelardi M et al. (2025) “Efficacy of dietary modifications and mucosal protectors in the treatment of laryngopharyngeal reflux: a multicenter study.” Frontiers in Medicine, 12:1488323. PMC
- Lechien JR et al. (2025) “Effectiveness of Diet Recommendations for Laryngopharyngeal Reflux Disease: A Systematic Review.” Journal of Voice. ScienceDirect
- McGlashan JA et al. (2009) “The value of a liquid alginate suspension (Gaviscon Advance) in the management of laryngopharyngeal reflux.” Journal of Laryngology and Otology. PubMed
- Wilkie MD et al. (2018) “Gaviscon Advance alone versus co-prescription of Gaviscon Advance and proton pump inhibitors in the treatment of laryngopharyngeal reflux.” European Archives of Oto-Rhino-Laryngology, 275(10):2515-2521. PubMed
- Koufman JA, Johnston N. (2012) “Potential Benefits of pH 8.8 Alkaline Drinking Water as an Adjunct in the Treatment of Reflux Disease.” Annals of Otology, Rhinology and Laryngology, 121(7):431-434. PubMed
David Gray
Content Researcher & Author
David Gray founded Wipeout Reflux to address a critical gap in reflux management. His research synthesizes over 100 peer-reviewed studies on laryngopharyngeal reflux (LPR), pepsin biology, and GERD pathophysiology. For LPR specifically—a condition most physicians misdiagnose—his work focuses on pepsin reactivation and why standard PPI therapy fails most patients. He develops evidence-based protocols targeting root causes of both LPR and GERD, integrating emerging research on sphincter dysfunction, dietary interventions, and newer clinical approaches. Wipeout Reflux represents practical application of clinical science for patients seeking real solutions.

Thanks for your working putting all this out. I have recently developed both GERD and LPR (really horrible symptoms and I am hypersensitive so feel everything 5x more than others).
Now, I have a conundrum, and I’m sure you’ll have an answer.
If my food portions are smaller for better digestion and not overfilling stomach (and normally they already were cos I’ have a tendency to hypoglycaemia) then I eat about 5 times a day. And maybe one snack (fruit) . But Gaviscon says we should keep it to 3x times a day after meals and 1x before bed. What about other meals? I have main 3 and the others are a bit smaller but not that much…. any suggestion?
Also a question where do you stand on avocado? it seems soothing but I don’t know if the amount of fats in them is bad…
Really appreciate that, and I totally relate to the hypersensitivity side of this — when your nervous system is dialed up, reflux symptoms can feel 10x worse.
Honestly, I think smaller, more frequent meals are often better for a lot of people with reflux/LPR than forcing 3 large meals. Overfilling the stomach is a huge trigger for many people. You don’t necessarily need to take Gaviscon after every tiny snack — a lot of people focus more on the bigger meals and before bed, since nighttime reflux is often the biggest issue.
As for avocado, I think it’s one of those very individual foods. Some people tolerate it really well and find it soothing, while others react because of the fat content. Personally, I’d just test a small amount and judge based on your own symptoms rather than assuming it’s automatically bad.
I assume that Gaviscon, like most other things, is not meant for long term use. Does the company say or do you know what the recommended term for use is (meaning Pepcid for example says do not use more than 2 weeks unless directed by a doc). Also – is there any information on negative effects Gavison does to your system?
BTW – I saw your response to the person who’s story related to seeing a functional medicine doc and the natural supplements they used to treat various things. You asked if he could share what they gave him. I too gave up on my GI and sought the help of functional medicine. They helped me with all of the things he mentioned (almost identical) and I was doing very well until a few months ago and now the sour burning mouth is back. I am actually feeling a bit lost at the moment because I think functional medicine has done all they can for me and I don’t want to go back to a GI. I would gladly share what things I used but I am not sure it would help as each has its own purpose. For example, my GI map showed H Pylori but unless you have that, what they prescribed would not help. They did not have any solutions related directly to reflux or LPR.
I think Gaviscon is relatively safe for long term use. It’s basically a mixture of alkaline minerals and the alginate from seaweed. So it’s basically natural. Unlike h2 blockers and PPIs which are man made and more troublesome long term. I personally would feel a lot better taking it long term that any of the other acid supressing medications. Sure you can let me know some of the things you tried it could help others and myself have some new ideas too.
Hi a gave birth and at my 4 week postpartum I woke up with swollen face hives and closing throat I thought it was allergy but then gradually after few days I felt like good stuck in my throat that even my voice was gone gradually I felt constant heartburn.
During postpartum I also took pain killers which I think contributed to my Gerd . Since I also felt. Like even water was not easily passing down my esophagus they perform a barium swallow which everything was fine only gastroesiphageal reflux noted during the test.
Also my endoscopy came out I had inactive mild gastritis. Every morning I wake up and start walking I start having sort of shortness of breath but in reality it feels like my throat is irritated because doctors did an asthma test and it came out good and other tests too . So the itchy irritated throat is still going on every day.
Dr put me on omeprazole 40 mg since august 2 but I don’t see improvement , today is September 18 and I feel desperate and like it will never go away! Symptoms are irritated throat and left side chest pain doctors haven’t diagnosed me with LPR but in some weeks I’ll go perform a acid monitoring test any advise?
The best thing to do is a low acid diet like my wipeout diet plan. On top of it look into Gaviscon advance or reflux gourmet to be taken after meals and at bedtime.
Did you ever feel you were getting better, then you are back to burning throat, this LPR is so exhausting, did you have burning throat for two years. Gaviscon A
helps. Did you take any vitamins.
Can you still be healing if you still get burning throat but not as often, how long after your two years did you feel that you were healing.
Is MCT ok and turmeric
Yeah I have that that experience before. I find keeping a food diary and general diary on these things can help you figure out what some of your triggers may be that may cause or worsen the bad days. I didn’t take any vitamins no.
It’s hard to say for sure but you could be healing if the burning is minimal, that perhaps is past refluxed pepsin in your throat tissues. Once I started doing the things that helped such a a low acid diet I noticed a difference rather quickly.
Turmeric is fine yes as long as it’s cooked. MCT I am not certain on, but if it was me I would avoid.
Hi David,
Giving an update – may help others. Prior to this reflux I had some diarrhea and more flatulence than normal. I changed some eating and then starting eating bread & rice (binding foods). Things quieted down and firmed up. Then this all happened. As most know, the doctors haven’t been any help. (ENT, GP, Pulmonary, GI, Cardiologist)
I am now seeing a functional medicine doctor. First words were – you may have something going on in gut. He was the first doctor to put his hands on me & said I have inflammation throughout my body. First up – GImap fecal test. Confirmation of h-pylori, strep & leaky gut, gluten problems. The GI doc had said no h-pylori during endo/colon-scopies.
Over the years I was having some issues and I ate good food. I got the “don’t eat this” list (all good foods) from doc with no further explanation. It was not getting better so I started eating bad food.
Following were those all too familiar symptoms – sinus, swollen throat, etc. Sent for allergy test – negative. They gave me antibiotics. Antibiotics can mess up the gut & may have caused more problems.
Next up – food test. I have numerous problems with many foods. Wheat, milk, bread, sugar, fruits, veggies & many more. About 70 foods.
The plan – I have been taking natural stuff to rid of the GI infection problems and will now have to alter my diet to get rid of the inflammation.
Now here is one of the most important things – most of the food in your plan is actually causing ME problems. I am back to where I started with good food causing problems, but finally have a doctor that is listening to me & getting proper tests to help.
I got a chest checkup on my own, a CAT scan. Lungs good, plaque in heart. Cardiologist – statin, statin. Me – no, I’ll see the doctor I am seeing now who sends me for CAC scoring test – yes, I have a minimal amount, but nothing to worry about. (Vitamins can help that later if needed) Reflux causing stress in area – reason many think they are having heart attacks.
Your site has been very helpful & got me on the path to correcting things. You did more for me to quiet down my throat than all those doctors I saw. Dr Aviv mentions inflammation, but never mentions each person may have different foods causing problems. It is not acid for me that is causing the problems.
Perhaps some of this information will help others.
I probably won’t be back to the site unless it’s another update, if you’d be ok with that.
Hi See,
Thank you for your story and the update it sounds like you are doing better now which is great to hear and I am happy to have been of a help to get you on that right track.
Yeah that’s an important thing to note, about how different foods and drinks can be triggers for different people and it’s important to keep that in mind even when doing a diet tailored for acid reflux.
One thing I wanted to ask you was about the GI infections and you mentioned you took natural stuff to improve it, what was that if you don’t mind sharing as I would be interested to know what worked for you.
Hello. So far after 6 months, LPR is slowly destroying a previously very healthy and good life. I can’t imagine not eating so many healthy foods and can’t imagine the nutritional deficiencies that would result from following this diet for life. That being said, I finally got desperate enough that I followed the diet for about 2 weeks strictly, then another 2 weeks with some non compliance at restaurants a few times. I was also following the advice of Dr. Kaufman (sp?), including taking pepsid a bunch of times daily with gaviscon advanced. I started feeling about 80% better but then the second I started reducing the pepsid, my acid reflux was far worse than before I started. She’s too expensive to continue consulting. But she said pepsid is much safer than PPIs (and she warns that PPIs cause acid rebound). But I’ve read several sources online that claim pepsid causes acid rebound. Have you had that experience? I really don’t know what to do. Pepsid is not safe long-term bc it interferes with nutritional absorption and other problems. Also, I didn’t have this mouth burning before I started the pepsid. It’s like the lump in throat improved, but the mouth burning started and really sucks. Do you know what exactly is causing the mouth burning? Also do you sleep at an incline? I have tried countless tactics to get comfortable and can’t. I have an adjustable bed now, and I can handle a couple of hours at 45 degrees (which she said is necessary — any lower incline doesn’t help). But then my lower back hurts too much to continue. I can’t handle the entire bed at all angle. I’ve tried. I have knee support but still my lower back can’t handle more. Did you get better sleeping flat? Do you sleep flat now? I probably have tons more questions but I haven’t been sleeping so I can’t remember. I will post later if I think of them. Thanks very much!
Yes rebound is still possible with H2 blockers like pepcid, though PPIs are usually the worst culprit. Yeah I had bad rebound before multiple times. I’d recommend you read my article on acid rebound here – Acid rebound. It’s probably the pepsin that comes up from the stomach causing the mouth burning would be my assumption. I have used a wedge pillow and haven’t found it to make much of a difference. Higher is better but it’s also more uncomfortable as I know myself. I think the wedge pillow is more useful for people with GERD symptoms not really LPR because the incline doesn’t help as much for LPR as its gaseous reflux not liquid like GERD. I sleep on a small incline now.